Academic Editor: Luigi Santacroce
The fracture of endodontic instruments inside the canal represents a problem that is not always easy to solve. The reutilization of endodontic instruments after sterilization procedures raises the question of how these processes affect their physical and mechanical properties. Alterations can involve the surface of the instruments, as well as their cutting effectiveness, shape and resistance to torsional and cyclic fatigue. The methodology adopted for this systematic review followed the PRISMA guidelines for systematic reviews. The following search terms were used in PubMed and Scopus: “endodontic sterilization”, “endodontic autoclave”, “cyclic fatigue”, “torsional”, “cutting efficiency”, “sterilization”, “surface characteristics” and “corrosion”. After the screening phase, the application of exclusion criteria and the removal of duplicates, 51 studies were identified and divided into four outcomes: cyclic fatigue; deformation and torsional fatigue; corrosion or surface alterations; and cutting efficiency. Our study of the scientific literature highlights disagreements between studies on these effects. After autoclaving, instruments exhibit a reduction in the cutting efficiency, but NiTi alloy instruments have an improved resistance to cyclic and torsional fatigue.
Over time, manufacturers have progressively perfected methods for the production of endodontic instruments for scouting, pre-flaring [1], preparing the glide path and shaping the endodontic canal [2]. Every endodontic file with a cutting capacity can also be employed for shaping. Here, the term “shaping step” refers to the shaping of the coronal, medium and apical parts following the scouting, pre-flaring and glide path steps [3].
The main steps of endodontic treatment are scouting, pre-flaring, glide path production, canal shaping and canal finishing, and each step requires an instrument that has different features that correspond to different physical and mechanical characteristics [4].
The sterilization process includes several phases: pre-sterilization, drying, packaging, heat sterilization and storage of the sterile material [5].
Pre-sterilization is the disinfection, decontamination and cleaning of dental instruments. This phase involves immersing the instruments in decontaminating and disinfecting liquids or cleansing them with washer-disinfectors. Decontamination reduces the microbial load on endodontic instruments, while cleansing removes organic and inorganic residues (to avoid the removal of debris by hand brushing, the use of ultrasonic trays is recommended) [6].
The subsequent phases involve the rinsing, drying and packaging of instruments, followed by heat sterilization (autoclave at 134 degrees at 2 atmospheres) to eliminate spores. The last phase is the storage of the instruments.
Other sterilization procedures after the pre-sterilization phase include glass bead sterilization or treatment with 2% glutaraldehyde (glutaraldehyde was used for high-level disinfection instead of sterilization but is not recommended because of its toxicity) [7].
An important limit to the reuse of endodontic instruments after sterilization lies in the inability to perfectly clean the blades from the debris created following the canal shaping phase [8]; the removal of debris by manual cleaning or with the help of ultrasonic trays does not allow to remove all debris of an organic and inorganic nature. And among these the prions which represent one of the contaminants that can resist decontamination procedures and are only partially inactivated and denatured at the temperatures reached by autoclaves used in dentistry; remember that prions are responsible for spongiform encephalopathy disease in humans [9, 10, 11, 12].
Walker et al. [13] in 2007 they described the theoretical possibility of transmission of the pathology through prions through dental and endodontic procedures, indicating however low the risk of transmission [13, 14, 15]. Contamination by prions would potentially be triggered by the contact of the blades of the endodontic instruments with the pulp nerve tissue [16]; In addition, in patients with spongiform encephalopathy prions can be found at the trigeminal level, as demonstrated by Guiroy et al. [17, 18].
The WHO guidelines report the following methods as methods for the inactivation of the prion and its denaturation, as reported by Walker et al. [13]:
These methods alter the surface of the instruments and are not applicable to dental endodontic instruments as reported by Sonntag et al. [20].
The fracture of endodontic instruments inside the canal is a problem that is not always easy to solve [21, 22, 23]. The potential reuse of many endodontic instruments after sterilization procedures raises the question of how much these processes influence their physical and mechanical properties. There are three possible answers to this question: the instrument properties deteriorate, improve or are unaffected [24].
Some studies suggest that sterilization procedures have no influence on these
instruments, but the results in the literature do not always agree. For example,
D. Zhao et al. [25] reported an increase in the cyclic fatigue
resistance of HyFlex CM, Twisted File and K3XF instruments (autoclave
sterilization was performed at 134
Thus, the literature reports conflicting findings about changes in endodontic instruments after sterilization procedures. These disagreements may be due to the multitude of instruments and methods used in endodontics and the different methods of sterilization and disinfection [32].
The heterogeneity of the results of the various studies could also depend on the high heterogeneity of the measurement apparatuses, in particular for the measurement of cyclic fatigue, Plotino [33] reports in a 2009 literature review as an ideal hypothetical model the curved canals of natural teeth, but the problem as set out by the author of the review and in the standardization of measurement.
All instruments for the measurement of cyclic fatigue that reproduce the artificial canal through a curved cylindrical tube are subject to wear and the endodontic instruments used within them have a degree of freedom following an unpredictable trajectory and without a precise measurement of radius and angle of curvature. In the realization of the measuring apparatus for cyclic fatigue, both the angle and the radius of curvature of the artificial canal are fundamental, which differ in the various studies on the resistance to cyclic fatigue [33].
NiTi endodontic instruments consist of a crystalline lattice with a body-centered cubic shape which takes the name of austenite which, following thermal variations or the application of forces, becomes a monoclinic structure called martensite [34].
For NiTi alloys the martensitic transformations are of the displastic type, obtained by cooling the austenitic phase with the release of heat [35]. The transformation from austenite to martensite consists of 2 moments: in the first we have all the atomic movements necessary to produce the new structure and in the second the adaptation of shape and volume with a change in the crystal lattice that can take place with the slip, which is permanent, or the twinning which is reversible (and is preferable if you want to get a return of shape) [36].
Following a lowering of the temperature which varies according to the type of alloy, the crystal lattice acquires an easily deformable martensitic type configuration, with a low yield point; while upon heating, the alloy forms an austenitic lattice [37]; Under the application of a force, the austenitic alloy behaves in a similar way, passing to a martensitic crystalline form through an intermediate transformation phase that can accommodate greater stress without increasing the tension. Therefore, an endodontic instrument while working inside the endodontic canals is subjected to deformation forces in which there is the transition from the austenitic to martensitic phase through a transformation phase. In the transformation phase, the instrument will show superplasticity characteristics before reaching the martensitic phase which could be followed by yielding and rupture [38, 39].
Previous studies on the subject by the same research group have focused on the torsional property and surface alterations of endodontic instruments subjected to sterilization, focusing neither on cyclic fatigue nor deformation [7, 40, 41]. To date, no other systematic reviews have addressed these topics (cyclic fatigue, deformation, torsional fatigue, corrosion or surface alterations, cutting efficiency) in relation to sterilization.
The purpose of this review is to provide the widest and most up-to-date overview of the topic through a systematic methodology involving the screening and selection of articles [42, 43]. Our hypothesis is that not all alterations induced by the autoclave have a negative effect on rotating endodontic instruments.
The following systematic review was performed in accordance with the PRISMA protocol (Preferred Reporting Items for Systematic reviews and Meta-Analyses): the outcomes, the data extraction process and the methods for their quantitative and qualitative synthesis were previously agreed upon by 3 reviewers.
The protocol and methodology adopted for this review have been used for previous systematic reviews by the same research group.
Articles that were eligible for inclusion in this review were in vitro or clinical studies that evaluated the influence of disinfection and sterilization procedures on rotary endodontic instruments and endodontic files. Reports that were not written in English, were published before 1980 or were published in journals of national interest only were excluded. We selected only articles published in the last 4 decades because the instruments and sterilization methods have profoundly changed. Four research outcomes were defined:
The studies were identified through bibliographic searches in electronic databases and the manual review of the biobibliography of previous systematic reviews conducted on the subject.
The literature search was conducted in the “PubMed” and “Scopus” search engines. The original search was conducted between 12.12.2020 and 01.03.2021, and a final search was conducted on 10.04.2021 for a partial update of the records.
We searched for different terms using the following combinations: “Endodontic sterilization” “endodontic autoclave” “cyclic fatigue” AND “sterilization”; “torsional” AND “sterilization”; “cutting efficiency” AND “sterilization” “surface characteristics” AND “sterilization”; “Corrosion” AND “sterilization”. Bibliographic citations of previous systematic reviews on the subject were also analyzed. Table 1 describes the research methodology for keyword searches in databases and article selection.
| Category | Exclusion criteria | Inclusion criteria |
| Publication language | Not English | English |
| Study type | Reviews, systematic reviews , case reports, case series, | in vitro studies |
| Data characteristics | I. Articles that do not report data on physical and mechanical characteristics (resistance to cyclic and torsional fatigue, alterations of the surface of the instruments, cutting efficiency) following sterilization procedures; | A. To include all studies reporting data on cyclic and torsional fatigue after sterilization; |
| II. To exclude all studies that measured the variation in resistance to torsional and cyclic fatigue as well as surface alterations and cutting efficiency after shaping procedures of artificial or natural canals. | B. To include all studies that report data on the variation of the topographical surface after sterilization; | |
| C. To include all studies reporting data on cutting efficiency after sterilization. | ||
| Year of publication | Published before 1979 | Published after 1979 |
| further inclusion and exclusion criteria applied to the network meta-analysis | ||
| Data characteristics | I. To exclude those data and studies in which the sterilization procedure was performed not in an autoclave; | A. The cyclic fatigue measurement must have been performed with a curvature angle of 60 |
| II. To exclude those studies that report data without a control (instruments not subjected to autoclaving cycles or other sterilization procedures); | degrees and a radius of curvature of 5 mm; | |
| III. To exclude all data on cyclic fatigue obtained on artificial canals with a curvature angle and a radius of curvature different from 60 degrees and 5 mm. | B. The sterilization procedure must have been carried out by means of an autoclave (10 cycles). | |
The “records” obtained from the search were subsequently screened by two independent reviewers (M.D. and D.S.). Situations of uncertainty or disagreement between the 2 reviewers were resolved by a third supervisor. Agreement between the 2 screening reviewers was measured by the K statistic, and K = 0.68.
After applying the preliminary eligibility criteria (articles in English and published after 1979) through the application of filters in search engines, duplicates were removed with the aid of the EndNote X8 software (Thomson Reuters , Clarivate Analytics, Philadelphia, PA, USA). Then, the two reviewers independently removed articles and studies that were not related to the topics of the review (endodontics and sterilization) by analyzing the title and abstract. The inclusion and exclusion criteria applied to the studies are shown in the Table 1.
Subsequently, studies were included in the qualitative analysis based on the 4 outcomes decided in advance.
The extraction of data from the included studies involved the development of tables and was performed by the two reviewers.
The characteristics of the data were the following: first author, date of publication, bibliographic reference, type of endodontic instrument, method of sterilization and alterations in the instruments induced by sterilization.
A total of 1195 records were identified in the PubMed and Scopus databases. After screening the articles through the use of filters (restriction by year and language), 996 articles were obtained, and 578 were retained after the removal of duplicates. After the application of the eligibility criteria (all articles relating to the topic of sterilization in endodontics), we arrived at 161 articles, and 103 articles remained after the elimination of duplicates. After the application of exclusion and inclusion criteria, we obtained 51 articles, which were divided according to the topics of interest: outcome 1 (16 studies that investigate the influence of disinfection and sterilization procedures on resistance to cyclic fatigue); outcome 2 (7 articles investigating the influence of disinfection and sterilization procedures on resistance to torsional fatigue); outcome 3 (23 articles investigating the effects of sterilization and disinfection on the surface characteristics of endodontic instruments); outcome 4 (7 articles investigating changes in the cutting efficiency of instruments after sterilization and disinfection procedures). Some articles were included in multiple outcomes.
The studies included in the quantitative analysis were as follows. First outcome: Khabiri et al. 2017 [27], Arias et al. 2014 [44], Zhao et al. 2016 [25], Plotino, et al. 2012 [45], Mize et al. 1998 [46], Viana et al. 2006 [26], Sharroufna and Mashyakhy, 2020 [47], Das et al. 2019 [48], Alshwaimi 2019 [49], Arias et al. 2020 [50], Kim et al. 2020 [51], Li et al. 2015 [52], Yang et al. 2018 [53], Pedullà et al. 2011 [54], Bulem et al. 2013 [55], Özyürek et al. 2017 [56],Second outcome: Iverson et al. 1985 [57], Chenail et al. 1986 [58], Hilt et al. 2000 [59], Silvaggio et al. 1997 [28], Canalda-Sahli et al. 1998 [60], King et al. 2011 [30], Casper et al. 2011 [29]. Third outcome: Razavian et al. 2016 [61], Alexandrou et al. 2005 [62], Qaed et al. 2018 [63], Li et al. 2015 [52], Alexandrou et al. 2006 [64], Yang et al. 2018 [53], Yılmaz et al. 2017 [65], Nair et al. 2015 [66], Valois et al. 2008 [67], Spagnuolo et al. 2012 [68], Inan etal. 2007 [69], Can Saglam et al. 2015 [70], Das et al. 2019 [48], Cai et al. 2017 [71], Prasad et al. 2014 [72], Saglam et al. 2012 [73], Topuz et al. 2008 [74], Ametrano et al. 2011 [75], Fayyad and Mahran [76], Uslu et al. 2018 [77], Shahi et al. 2012 [78], Stokes et al. 1999 [79], Casella et al. 2011 [80]. Fourth outcome: Schafer et al. 2002 [81], Haikel et al. 1996 [82], Rapisarda et al. 1999 [31], Seago et al. 2015 [83], Haikel et al. 1998 [84], Morrison et al. 1989 [85], Neal et al. 1983 [86]. There are 4 articles included in the network meta-analysis for the first outcome: Sharroufna and Mashyakhy, 2020 [47], Kim et al. 2020 [51], Özyürek et al. 2017 [56], Plotino, et al. 2012 [45].
The entire selection and screening procedure, as described in Table 2 (Ref. [7, 40, 41, 87, 88, 89, 90]), is presented in the flowchart in Fig. 1.
| Database - Provider | Key words and search details | Number of records | Number of records) after restriction by year of publication and language (last 40 years) | After remove overlaps articles | Number of remaining articles after screening for the latest review topic | Article remaining after application of the inclusion and exclusion criteria |
| Pub-med | Search: “endodontic” AND “sterilization” Sort by: Most Recent | 224 | 161 | |||
| “endodontic” [All Fields] AND “sterilization” [All Fields] | ||||||
| Pub-med | Search: “endodontic” AND “autoclave” Sort by: Most Recent | 45 | 42 | |||
| “endodontic” [All Fields] AND “autoclave” [All Fields] | ||||||
| Pub-med | Search: “cyclic fatigue” AND “sterilization” Sort by: Most Recent | 29 | 27 | |||
| “cyclic fatigue” [All Fields] AND “sterilization” [All Fields] | ||||||
| Pub-Med | Search: “torsional” AND “sterilization” Sort by: Most Recent | 34 | 31 | |||
| “torsional” [All Fields] AND “sterilization” [All Fields] | ||||||
| Pub-med | Search: “cutting efficiency” AND “sterilization” Sort by: Most Recent | 17 | 17 | |||
| “cutting efficiency” [All Fields] AND “sterilization” [All Fields] | ||||||
| Pub-med | Search: “surface characteristics” AND “sterilization” Sort by: Most Recent | 34 | 33 | |||
| “surface characteristics” [All Fields] AND “sterilization” [All Fields] | ||||||
| Pub-med | Search: “Corrosion” AND “sterilization” Sort by: Most Recent | 151 | 107 | |||
| “Corrosion” [All Fields] AND “sterilization” [All Fields] | ||||||
| Scopus | TITLE-ABS-KEY (endodontic AND sterilization | 301 | 229 | |||
| Scopus | TITLE-ABS-KEY (“endodontic” AND “autoclave”) | 64 | 60 | |||
| Dioguardi et al. 2021 [88] | Systematic review | 65 | 62 | |||
| Silva et al. 2020 [87] | Systematic review | 40 | 40 | |||
| Dioguardi et al. 2020 [7] | Systematic review | 97 | 95 | |||
| Jena et al., 2020 [89] | Review | 25 | 24 | |||
| Dioguardi et al. 2019 [40] | Systematic review | 28 | 28 | |||
| Rajpurohit and Chowdary, 2019 [90] | Review | 16 | 16 | |||
| Dioguardi et al. 2019 [41] | Systematic review | 25 | 24 | |||
| Total records | 1195 | 996 | 578 | 103 | 51 |
 Fig. 1.
Fig. 1.Flowchart of the different phases of the systematic review.
Cyclic fatigue is one of the main causes of fractures of rotating instruments made of NiTi. With the advent of new NiTi alloys and the introduction of new production methods, the occurrence of cyclic fatigue has been increasingly reduced [36, 91, 92, 93]. NiTi alloys today have equal atomic concentrations, which renders the austenitic phase very stable. A change in the proportion between titanium and nickel makes the alloy more unstable, and transformation into the super-elastic martensitic phase is favored under stress. After the super-elastic martensitic phase, the instrument undergoes compression and bending cycles, as is usually the case for instruments rotating in curved canals, after which it deforms and breaks [92, 94, 95]. The studies in the literature can be divided into two subgroups: those that investigated the effects of hypochlorite on cyclic fatigue (Table 3, Ref. [54, 55]) and those that investigated the effects of hot sterilization procedures on cyclic fatigue resistance (Table 4, Ref. [25, 26, 27, 44, 45, 46, 47, 48, 49, 50, 51, 52, 53]).
| Autor, data | Instruments | Sterilization methods | Influence on resistance to cyclic fatigue |
| Pedullà et al. 2011 [54] | Twisted Files, Revo S, Mtwo files | 5% NaOCl solution | No influence |
| Bulem et al. 2013 [55] | ProFile, FlexMaster, Mtwo and TwistedFiles | immersed in NaOCl; immersed in NaOCl and sterilized in one autoclave cycle; 5 cycles immersed in NaOCl and sterilized in autoclave and not immersed in NaOCl and not sterilized | No influence |
| Autor, data | Instruments | Sterilization methods | Influence on resistance to cyclic fatigue in relation to sterilization cycles |
| Khabiri et al. 2017 [27] | 90 Nickel-Titanium 642 rotary files #30 with 0.06 tape | 134 |
No influence |
| Arias et al. 2014 [44] | GT, GTX files | immersed in NaOCl and Autoclave | Increase resistance |
| Zhao et al. 2016 [25] | HyFlex CM, TF and K3XF | autoclave sterilization was performed at 134 |
Increase resistance |
| Plotino, et al. 2012 [45] | K3, Mtwo, Vortex, and K3 XF | autoclave | Increase resistance (only k3 XF) |
| Mize et al. 1998 [46] | Ni-Ti instruments | 135 |
No influence |
| Viana et al. 2006 [26] | ProFile | Dry heat sterilization cycles 170 |
Increase resistance |
| Sharroufna and Mashyakhy, 2020 [47] | EdgeFile X7, Vortex Blue, TRUShape | autoclave sterilization (10 cycles) at a temperature of 134 |
Increase resistance (only EdgeFile X7) |
| Das et al. 2019 [48] | Hyflex CM, Hyflex EDM | autoclave sterilization at 121 |
Not applicable |
| Alshwaimi 2019 [49] | Proflexendo rotary files | 134 |
Reduced the cyclic fatigue resistance of Proflexendo files |
| Arias et al. 2020 [50] | Hyflex EDM, TRUShape | 136 |
Gamma-irradiation decreased cyclic fatigue resistance of TRUShape; sterilization decreased fatigue resistance Hyflex EDM |
| Kim et al. 2020 [51] | ProTaper Universal, K3XF, HyFlex EDM, and TF adaptive | autoclave (10 cycles) 132 |
No influence |
| Li et al. 2015 [52] | K3, Mtwo, ProTaper | 134 |
Increase resistance |
| Yang et al. 2018 [53] | K3XF, K3 | autoclave | No influence |
The studies conducted by Pedullà et al. [54] and Bulem et al. [55] agree that 5 percent sodium hypochlorite has no influence on cyclic fatigue, neither worsening nor improving it, regardless of whether the chemical is used as a canal irrigant or as a disinfectant agent for the instruments.
Other studies that support a lack of influence on cyclic fatigue are those conducted by Mize et al. [46], Khabiri et al. [27] and Kim et al. [51]. In these studies, there was no statistically significant increase or decrease. The investigated instruments were a Profile rotary file, ProTaper Universal, K3XF, HyFlex EDM and TF adaptive.
Conversely, other studies describe an increase in resistance to cyclic fatigue for the K3, K3XF, Mtwo, ProTaper, GT, GTX, Vortex, EdgeFile X7 and Twisted file instruments [26, 45, 47, 52].
In contrast to these data, Alshwaimi [49] report a reduction in resistance to cyclic fatigue for Proflexendo rotary files. A decrease was also found for HyFlex EDM in a study by Arias et al. [50].
There is an apparent contrast among the results of different studies. Thus, for a definitive analysis, a meta-analysis should be carried out by extracting data from reports, such as the average number of cycles to failure and the length of fragments. However, there is excessive diversity in the studies, such as different apparatuses to measure cyclic fatigue, different angles of curvature of the artificial canals with which the cyclic fatigue was measured, the heterogeneity of instruments and different numbers of sterilization cycles. These differences can lead to results with a high heterogeneity index, as also indicated by a recent systematic review conducted by Silva et al. [87].
In light of the high heterogeneity of the instruments investigated and of the investigation methods that are not always standardized (variations in the radius and angle of curvature), the 2 reviewers decided not to perform a meta-analysis of the data (variation in the number of cycles upon failure after sterilization) comparing instruments never autoclaved and instruments with 10 autoclave cycles, but to perform a Network meta-analysis comparing the different endodontic instruments through an indirect and direct comparison of the various rotating instruments. The data included in the network meta-analysis (mean difference, of the variation of the Number of Cycles to Failure) respects the principle of similarity (only the studies that reported data on NFC on non-sterilized instruments and after 10 sterilizations, obtained with artificial canals with a radius of curvature of 5 mm and a curvature angle of 60 degrees) since the methodology adopted is similar in each study and therefore comparable (Table 5, Ref. [45, 47, 51, 56]). The network diagram shown in Fig. 2 shows us how the main data of the direct comparisons are mainly on the K3XF, Vortex and PTU nodes with a similar robustness of the lines towards the various nodes.
| Intruments | Cycles autoclave | Number | N.C.F. | S.D. | Mean difference | S.D.M.D. | |
| Sharroufna and Mashyakhy, 2020 [47] | EFX7 | 0 | 12 | 755.8 | –443.0 | 219.2 | |
| 10 | 12 | 1198.8 | |||||
| Vortex | 0 | 12 | 568.7 | –37.4 | 160.53 | ||
| 10 | 12 | 606.1 | |||||
| TS | 0 | 12 | 442.2 | 45.6 | 80.8 | ||
| 10 | 12 | 487.8 | |||||
| Kim 2020 [51] | PTU | 0 | 10 | 1712.9 | 270.1 | 330.26 | |
| 10 | 10 | 1442.8 | |||||
| EDM | 0 | 10 | 11645.3 | –290.6 | 1702.75 | ||
| 10 | 10 | 11935.9 | |||||
| TFA | 0 | 10 | 1344.7 | 78.7 | 330.71 | ||
| 10 | 10 | 1266.0 | |||||
| K3XF | 0 | 10 | 1726.8 | 473.9 | 329.99 | ||
| 10 | 10 | 1252.9 | |||||
| Plotino et al. 2012 [45] | K3 | 0 | 12 | 439 | 15 | 54.52 | |
| 10 | 12 | 424 | |||||
| Mtwo | 0 | 12 | 419 | 10 | 48.09 | ||
| 10 | 12 | 409 | |||||
| Vortex | 0 | 12 | 454 | –26 | 99.60 | ||
| 10 | 12 | 480 | 104 | ||||
| K3XF | 0 | 12 | 651 | –111 | 175.79 | ||
| 10 | 12 | 762 | |||||
| Özyürek et al. 2017 [56] | PTG | 0 | 20 | 1045.21 | –261.13 | 224.62 | |
| 10 | 20 | 1306.34 | |||||
| PTN | 0 | 20 | 525.44 | –98.82 | 104.09 | ||
| 10 | 20 | 624.26 | |||||
| PTU | 0 | 20 | 248.12 | –3.97 | 33.06 | ||
| 10 | 20 | 252.09 |
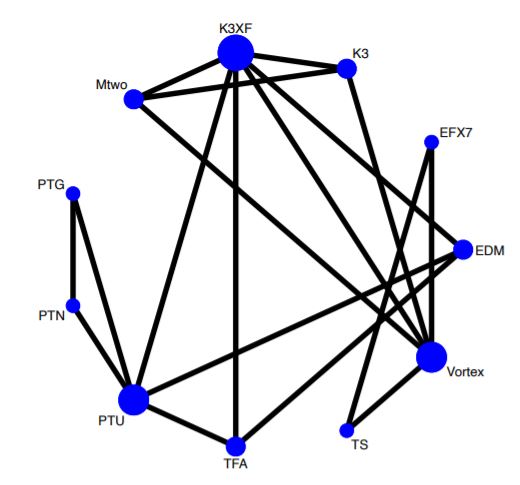 Fig. 2.
Fig. 2.Network geometry. The size of the 11 nodes, one for each treatment, indicates the number of studies included in the corresponding nodes, while the thickness of the lines connecting 2 nodes indicates the amount of relevant data (PTG, Protaper Gold; PTN, Protaper Next; PTU, Protaper Universal; TFA, TF adaptive file; TS, TRUShape; Vortex; EDM, HyFlex EDM; EFX7, EdgeFile X7; K3, K3XF, Mtwo).
The general consistency test reports at Chi
For the analysis of the effect size, we proceeded through the representation by forest plot Fig. 3.
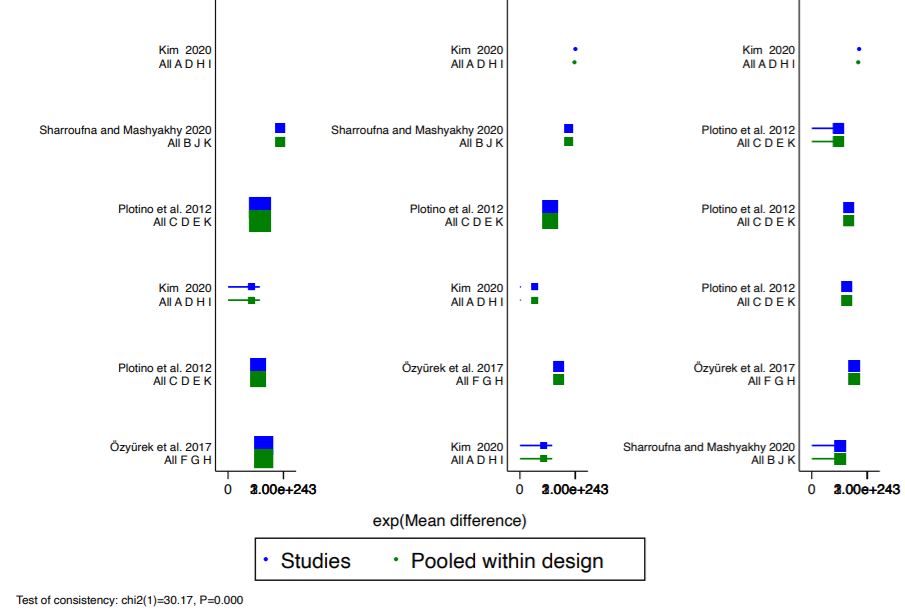 Fig. 3.
Fig. 3.Network Forest plot. All direct and mixed comparisons. A: EDM, B: EFX7, C: K3, D: K3XF, E: Mtwo, F: PTG, G: PTN, H: PTU, I: TFA, J: TS, K: Vortex.
We then evaluated the instruments that after 10 autoclave cycles exhibit the lowest reduction in the number of turns at failure as shown in Fig. 4 and Table 6, the probability that the EDM endodontic instrument is the best (with the least reduction of NFCs) is approximately 71.8% and the probability that it is at least the second best is 6.4%. In the SUCRA (surface under the cumulative ranking), in fact, the surface for the EDM instrument reaches almost 90%, while we have that the PTG endodontic instrument has the probability that it is the best is 20.4% and 51.2% that it is the second, with a SUCRA also of 90%.
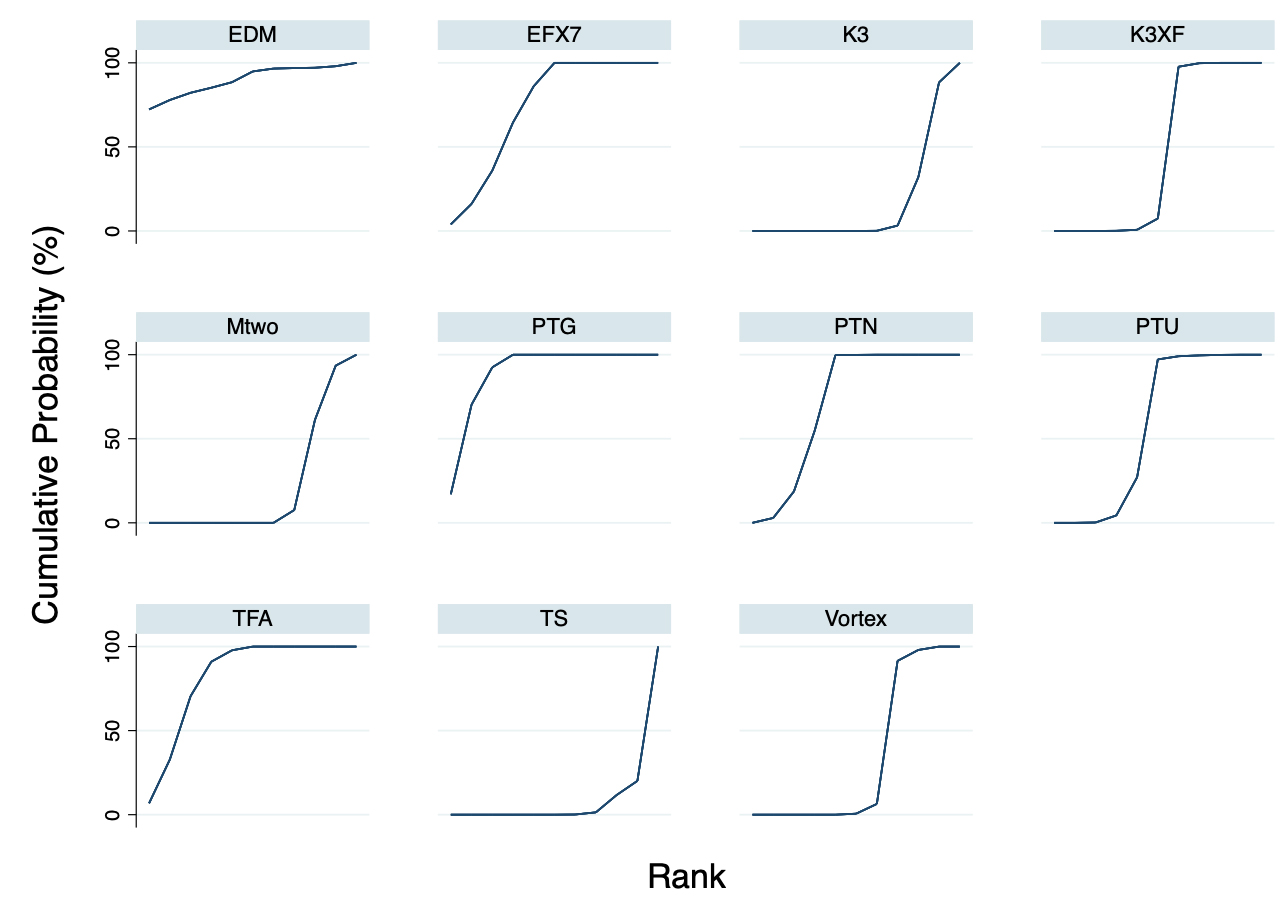 Fig. 4.
Fig. 4.Results of the network rank test. Graphical ranking; SUCRA: surface under the cumulative ranking. The higher the SUCRA value, the greater the probability that one instrument is better than the others with a lower reduction of NCFs after 10 cycles of sterilization.
| Rank | EDM | EFX7 | K3 | K3XF | Mtwo | PTG | PTN | PTU | TFA | TS | Vortex |
| Best | 71.8 | 2.4 | 0.0 | 0.0 | 0.0 | 20.4 | 0.0 | 0.0 | 5.4 | 0.0 | 0.0 |
| 2nd | 6.4 | 10.9 | 0.0 | 0.0 | 0.0 | 51.9 | 3.6 | 0.0 | 27.2 | 0.0 | 0.0 |
| 3rd | 4.1 | 20.3 | 0.0 | 0.0 | 0.0 | 21.5 | 16.7 | 0.7 | 36.7 | 0.0 | 0.0 |
| 4th | 2.7 | 29.5 | 0.0 | 0.0 | 0.0 | 6.2 | 36.8 | 4.7 | 20.1 | 0.0 | 0.0 |
| 5th | 1.9 | 21.7 | 0.0 | 0.4 | 0.0 | 0.0 | 42.8 | 24.1 | 9.1 | 0.0 | 0.0 |
| 6th | 7.2 | 15.2 | 0.0 | 7.6 | 0.0 | 0.0 | 0.1 | 68.3 | 1.5 | 0.0 | 0.1 |
| 7th | 1.8 | 0.0 | 0.0 | 90.0 | 0.1 | 0.0 | 0.0 | 1.9 | 0.0 | 0.2 | 6.0 |
| 8th | 0.7 | 0.0 | 4.2 | 2.0 | 5.7 | 0.0 | 0.0 | 0.2 | 0.0 | 1.6 | 85.6 |
| 9th | 0.3 | 0.0 | 31.2 | 0.0 | 53.5 | 0.0 | 0.0 | 0.1 | 0.0 | 9.1 | 5.8 |
| 10th | 0.4 | 0.0 | 53.2 | 0.0 | 34.0 | 0.0 | 0.0 | 0.0 | 0.0 | 9.9 | 2.5 |
| Worst | 2.7 | 0.0 | 11.4 | 0.0 | 6.7 | 0.0 | 0.0 | 0.0 | 0.0 | 79.2 | 0.0 |
| Mean rank | 2.2 | 4.0 | 9.7 | 6.9 | 9.4 | 2.1 | 4.2 | 5.7 | 3.0 | 10.7 | 8.0 |
| SUCRA | 0.9 | 0.7 | 0.1 | 0.4 | 0.2 | 0.9 | 0.7 | 0.5 | 0.8 | 0.0 | 0.3 |
Among the fundamental properties that an endodontic instrument must have in order to be safely used in the endodontic canal is torsion resistance.
Torsion is defined as the stress to which an elongated body is subjected when one of its sections is rotated with respect to another or the effect of such stress [96].
In the most up-to-date methods, instruments such as K-files, NiTi files, Unifile and flex-or-files (generally 2% tapered instruments) are used to explore the endodontic canal and execute the glide path [97]; These instruments must exhibit characteristics of flexibility and resistance to torsion and lt the end of each clinical use, it is important to inspect and eliminate instruments that have deformations or show stretching of the blades [98].
Iverson et al. [57] investigated the K-Flex and Burns Unifile instruments and reported that the torsion resistance of K-Flex files increased by 12.7% and 9.7% after heat and cold sterilization, respectively, compared with that of the controls and files subjected to other sterilization methods. These data are in contrast to the results reported by Chenail et al. [58], who studied the same instruments but observed no statistically significant influence, and agree with the findings of Hilt et al. [59], who reported no negative or positive influence on NiTi K-files.
These studies show that, for manual endodontic instruments with a constant taper of 2% made of both steel and nickel titanium (K-file, NiTi file), sterilization has neither a positive nor negative influence.
For rotary instruments, the torsional resistance of Profile instruments after sterilization was investigated for the first time by Silvaggio et al. [28] in 1997, who observed an improvement in resistance, and further studies on Twisted files and M-wire alloys also showed improvements [29, 36].
Alazemi et al. [99] reported that HyFlex instruments recovered their shape following clinical use and subsequent autoclaving.
Deterioration was only reported in one study, which was conducted by King et al. [30] on GT Series X files (Table 7, Ref. [28, 29, 30, 51, 57, 58, 59, 60, 99, 100, 101]).
| Autor, data | Sterilization methods | Instruments | Torsion resistance |
| Iverson et al. 1985 [57] | Hot sterilization | K flex, Burs unifile | Increase for burns unifile after 10 sterilization cycles |
| Chenail et al. 1986 [58] | Cold and dry heat sterilization | K flex, Burs unifile | No influence |
| Hilt et al. 2000 [59] | Hot sterilization | K file in acciaaio and in NiTi | No influence |
| Silvaggio et al. 1997 [28] | Hot sterilization | Profile | Increase resistance |
| Canalda-Sahli et al. 1998 [60] | Autoclaving | Nitiflex Naviflex Microtitane Flexofile Flex-R | Increase for NiTi |
| King et al. 2011 [30] | Autoclaving | Gt serie x twisted file | Reduction Gt serie x Increase twisted file |
| Casper et al. 2011 [29] | Autoclaving | Profile Vortex Twisted Files CM Wire file | Increase CM Mwire |
| Alazemi et al. 2014 [99] | Autoclaving | HyFlex CM | Form recovery after sterilization |
| Kim et al. 2020 [51] | Autoclaving | ProTaper Universal, K3XF, HyFlex EDM, and TF adaptive | No influence |
| Testarelli et al. 2003 [100] | Autoclaving 124 |
Hero | No influence |
| Haïkel et al. 2003 [101] | hot sterilization, 180 |
Unifile, Flexofile and H-File | No influence |
A recent systematic review of the literature conducted by this research group identified a meta-analysis of data on the variations in the deflection angle (the angle that is generated at the moment of fracture) and in the torsional moment of NiTi and steel instruments after sterilization procedures. The data reveal reductions in the torsional fatigue resistance (reduction of the torsional moment) and the deflection angle, but with low statistical significance. The authors of the review cite the high heterogeneity among the included studies as a limitation [40].
An undesired effect of heat sterilization (autoclave and dry heat sterilization) on the surface of instruments is the formation of surface irregularities or micro-pitting [102]. Corrosion can also occur following the use of sodium hypochlorite or other dental disinfectants [103].
In the reviewed literature, three types of methods were used to analyze the level of corrosion: atomic force microscopy (AFM) [66], scanning electron microscopy (SEM) [64] and electrochemical methods (saturated calomel electrode (SCE), open circuit potential (OCP) and Electrochemical Impedance Spectroscopy (EIS)) [78].
We divided the articles into three sub-groups and extracted the corresponding data, which are reported in three different tables.
SEM analysis showed the presence of topographical alterations on the surface. These alterations are already visible after the first autoclave cycle and can represent points where microcracks are induced in the structure, indicating cyclic or torsional fatigue failure.
Corrosion resistance is higher for alloys with equal atomic concentrations of nickel and titanium, and corrosion phenomena are more evident for alloys (46 titanium alloys, 56 nickel) with chromium inclusions, which facilitate corrosion through the formation of intermediate alloys [104].
Qaed et al. [63] observed these superficial alterations on AlphaKite and
Revo-S NiTi rotary files, with an increase in surface changes after three cycles
at a temperature of under 121
| Autor, data | Instruments | Sterilization methods | Results |
| Razavian et al. 2016 [61] | S-Files | 1, 5 and 10 autoclave | O = Debris and roughness |
| Cycles | 1 = No significant | ||
| 5 = Significant increase in roughness | |||
| 10 = Significant increase in roughness | |||
| Alexandrou et al. 2005 [62] | Mani NRT NiTi | 1, 6 and 11 autoclave | 1 = No significant |
| cycles | 6 = No significant | ||
| 11 = Significant increase in roughness | |||
| Qaed et al. 2018 [63] | Revo-S NiTi rotary | Control | show a smoother surface with few machining grooves |
| each instrument 3 shaped channels with a single autoclave cycle | dulling and blunting of the cutting edges is predominant | ||
| each instrument 9 shaped channels with a 3 autoclave cycle | showed plastic deformation, disruption in the surface with metal flakes | ||
| AlphaKite | control | gross machining grooves on their surface with no pits, strips or disruption | |
| each instrument 3 shaped channels with a single autoclave cycle | disruption of cutting edges | ||
| each instrument 9 shaped channels with a 3 autoclave cycle | microcracks, metal stripping | ||
| Li et al. 2015 [52] | K2, mtwo, protaper | 10 cycles of sterilization autoclave | surface and inner imperfections in all instruments were intensified greatly after 10 cycles of sterilization |
| Alexandrou et al. 2006 [64] | ProFile, Flexmaster | 11 autoclave cycles | Increased roughness was observed in all samples that were exposed to repeated sterilizations |
| Yang et al. 2018 [53] | K3XF, K3 | 10, 20 and 30 Autoclave cycles | The surface roughness of K3XF was increased after autoclave |
Studies on longitudinal sections were conducted by Alexandrou et al. [62], who noted a statistically significant increase in the surface roughness of NiTi instruments after 11 autoclave cycles. Moreover, SEM on the longitudinal sections of the inclusions and holes indicated a significant increase from 1 to 11 autoclave cycles [62].
The atomic force microscope consists of a cantilever with a sharp tip (tip) mounted on the end, typically composed of silicon or silicon nitride, which has a radius of curvature of the order of nanometers. Flexing the detector tip causes it to interact with the sample through van der Waals forces [105].
Three main parameters are taken into consideration when analyzing the surface with AFM: arithmetic mean roughness (AMR), maximum height (MH) and root mean square (RMS).
Data from studies conducted with atomic force microscopy are in agreement with those conducted with SEM. They report a statistically significant increase in surface imperfections after five autoclave cycles. The analyzed studies and their results are shown in Table 6. The corrosive effects of sodium hypochlorite and EDTA were studied using AFM by Uslu et al. [77], Prasad et al. [72], Cai et al. [71], Saglam et al. [73], Topuz et al. [74], Ametrano et al. [75], Fayyad and Mahran [76] and Can Saglam et al. [70] (Table 9, Ref. [48, 65, 66, 67, 68, 69, 70, 71, 72, 73, 74, 75, 76, 77]).
| Autor, data | Instruments | Sterilization methods | Results |
| Yılmaz et al. 2017 [65] | HyFlex EDM | 1, 5 and 10 autoclave cycles | Significant increase in roughness |
| Nair et al. 2015 [66] | Mani NRT NiTi, M two file | 1, 5 and 10 autoclaves cycles | Significant increase in roughness |
| Valois et al. 2008 [67] | Greater Taper, ProFile | 1, 5 and 10 autoclaves cycles | Significant increase in roughness |
| Spagnuolo et al. 2012 [68] | ProTaper, TiN -coated AlphaKite | 1, 5 and 10 autoclaves cycles | Significant increase in roughness |
| Inan et al. 2007 [69] | ProTaper | 1 autoclave cycles | Significant increase in roughness |
| Can Saglam et al. 2015 [70] | ProTaper retreatment, R-endo, and Mtwo | autoclaved five times and, 2% NaOCl or Chloroform | Surface alteration |
| Das et al. 2019 [48] | Hyflex CM, Hyflex EDM | autoclave sterilization at | Higher surface roughness |
| Cai et al. 2017 [71] | HyFlex, M3 | 5.25% NaOCl, 17% Edta | The surface roughness of 5.25% NaOCl and 17% EDTA immersed M3 files significantly increased compared to the control groups |
| Prasad et al. 2014 [72] | ProTaper and iRaCe | 5.25% NaOCl, 17% EDTA | Short-term contact with 17% EDTA and 5% NaOCl can cause significant surface deterioration |
| Saglam et al. 2012 [73] | ProTaper | 2.5% NaOCl, 5% NaOCl, 2% CHX, and MTAD | All tested solutions caused surface alterations |
| Topuz et al. 2008 [74] | RaCe | NaOCl solution for 5 min | NaOCl causes deterioration on the surface of RaCe |
| Ametrano et al. 2011 [75] | ProTaper | 5.25% NaOCl, 17% EDTA | short-term contact between NaOCl and EDTA endodontic irrigants and ProTaper instruments caused alterations in the surface of instruments |
| Fayyad and Mahran [76] | GTX, TF, RaCe and Hero Shaper | 5.25% NaOCl, 17% EDTA | 17% EDTA did not significantly affect the surface roughness of the instruments, whilst 5.25% NaOCl increased the surface roughness |
| Uslu et al. 2018 [77] | HyFlex EDM, HyFlex CM | 5.25% NaOCl, 17% EDTA | EDTA increase roughness, NaOCl not increase |
A previous literature review with meta-analysis conducted by our research group [41] was carried out on the surface alterations induced by autoclaving, sodium hypochlorite and EDTA. The AMR and RMS were used as parameters in the AFM analysis of the surface. The results suggest that five autoclave cycles induce statistically significant corrosive phenomena, called micro-pitting, and corrosion occurs after only 5 minutes of hypochlorite exposure and after 10 minutes of EDTA exposure [41].
The scientific literature is in full agreement that both intra-canal disinfectants and autoclave sterilization cause surface alterations.
Shahi et al. [78], Stokes et al. [79] and Casella et al. [80] used electrochemical systems to investigate the effects of hypochlorite on the surfaces of instruments. The specific methods with the results are reported in Table 10 (Ref. [78, 79, 80]).
| Autor, data | Means of investigation | Instruments | Results |
| Shahi et al. 2012 [78] | Electrochemical Impedance Spectroscopy (EIS) | RaCe, Mtwo | Corrosion resistance was significantly higher in Mtwo files compared to RaCe files in sizes #25, #30, and #35 and these properties might affect clinical efficacy of these instruments |
| Stokes et al. 1999 [79] | open circuit potential (OCP) (NaClO 5.25% for 1 Hour) | K-Flex, Flex-O, Flex-R, NiTifile | No significant difference between stainless steel and NiTi |
| Casella et al. 2011 [80] | saturated calomel electrode (SCE) 5% NaClO aerated solution at 37 uC | GT Rotary, K3, K file | The sterilisation treatment had no significant influence on the corrosion resistance (Only k3 decrease corrosion) |
According to these studies, immersion in sodium hypochlorite at concentrations equal to 5.25% at a temperature of 37 degrees does not cause a significant decrease in corrosion resistance, although both SEM and AFM reveal effects on the investigated surface, as previously reported. If the exposure times exceed 12–24 hours, the corrosive effects will be apparent not only microscopically but also macroscopically.
The first studies conducted on changes in cutting efficiency following sterilization were conducted by Neal et al. in 1983 [86], who described a significant decrease in the cutting capacity of K-files after 10 cycles of autoclaving. Subsequently, these data were partially disproved by Morrison et al. [85], who stated that there was no reduction in the cutting depth after five autoclaving cycles and that decreases were only due to clinical use.
Similar to Morrison, Seago et al. [83] did not observe any statistically significant reductions in the cutting capacity of HyFlex (rotary NiTi instruments) after one or two autoclave cycles.
Rapisarda et al. [31] reported that the cutting capacity of Profile NiTi rotary tools was reduced, with decreases ranging from 20% for 7 cycles to 50% for 14 cycles (heat sterilization). Corrosive phenomena were induced by the oxidation of surface layers with the formation of NiTi oxides [31].
The data reported by Schafer et al. [81] and Haikel et al.
[82, 84] support a reduction in cutting efficiency. Schafer observed a reduction
in the cutting efficiency of K-wires (NiTi) equal to 16.1% after 5 sterilization
cycles and 50.8% after 10 autoclaving cycles at a temperature of 135
The effects of heat sterilization can appear after 5 sterilization cycles, but in most studies, they became evident after 10 cycles [31, 81, 82]. Sodium hypochlorite with concentrations ranging from 2.5% to 5.25% for 30 minutes showed no effect on shear capacity, as reported by Schafer et al. [81], but if the duration reached 12–48 hours, corrosive phenomena were triggered, resulting in a net reduction in efficiency [84, 106] (Table 11, Ref. [31, 81, 82, 83, 84, 85, 86]).
| Author data | Instruments | Method sterilization | Reduction of cutting capacity, expressed as a percentage of the control |
| Schafer et al. 2002 [81] | Niti Kfile PVD | Autoclave 5–10 cycles 135° | No reduction |
| NaOC1 5.25% 30 minutes | No reduction | ||
| Niti Kfile | Autoclave 5–10 cycles | 50.6%–16.1% | |
| NaOC1 5.25% | No reduction | ||
| Haikel et al. 1996 [82] | Unifile | Dry hot sterilization 5–10 cycles 180° per 2 hours | No reduction (115.9%–104.9% efficacy) |
| NaOCl 2% 12–48 hours | 29.7%–36.7% | ||
| Ultrasonic cleaning 1–4 hours, NaOC1 (2.5%) and NH 4 (5%) | 61.8%–61.8% | ||
| NH4 1–4 hours | 62.6%–62.2% | ||
| Chemiclave 5–20 cycles per 20 minutes | 63.9%–67.1% | ||
| Glass bed sterilization 10–40 cycles per 40 seconds at 250° | 5.4%–14.1% | ||
| Flexofile | Dry hot sterilization 5–10 cycles per 2 hours 180° | 1.1%–1.7% | |
| NaOC1 2% 12–48 hours | 57.9%–67.6% | ||
| Ultrasonic cleaning 1–4 hours NaOC1 (2.5%) and NH 4 (5%) | 66.8%–65.7% | ||
| NH4 1–4 hours | 68.5%–68.5% | ||
| Chemiclave 5–20 cycles per 20 minutes | 77%–73% | ||
| Glass bed sterilization 10–40 cycles per 40 seconds at 250 |
67.4%–66.9% | ||
| H-File | Dry hot sterilization 5–10 cycles per 2 hours | 49.8%–54.1% | |
| NaOCl 2% 12–48 hours | 66.3%–62.9% | ||
| Ultrasonic cleaning 1–4 hours NaOC1 (2.5%) and NH 4 (5%) | 65.3%–97.8% | ||
| NH4 1–4 hours | 50%–53.5% | ||
| Chemiclave 5–20 cycles per 20 minutes | 68.1%–50.4% | ||
| Glass bed sterilization 10–40 cycles per 40 seconds at 250 |
76%–59% | ||
| Rapisarda et al. 1999 [31] | ProFile instruments | 7–14 cycles autoclave | 20%–50% |
| Seago et al. 2015 [83] | Hyflex CM NiTi rotary files | From 1 to 9 sterilization cycles by autoclave after each single use | no statistical decrease after 1, 4, 5, and 6 cycles. A statistically significant decrease in cutting efficiency was for 2, 3, 7, 8, and 9 cycles |
| Haikel et al. 1998 [84] | Niti file Maillefer | 2.5% NaOCI. 12–48 hours | (109.8% efficacy)–24.36% |
| Niti file Brasseler | 2.5% NaOCI. 12–48 hours | 16.42%–32.87% | |
| Niti file JS Dental | 2.5% NaOCI. 12–48 hours | 29.97%–25.35% | |
| Niti file McSpadden | 2.5% NaOCI. 12–48 hours | 3.25%- no reduction | |
| Morrison et al. 1989 [85] | K file | Sterilization after 1, 5, 10 use | No statistically significant change compared to the control group |
| Flexofiles | Sterilization after 1, 5, 10 use | No statistically significant change compared to the control group | |
| Neal et al. 1983 [86] | K-type, stainless steel files | autoclave sterilization resulted in a small but significant decrease in cutting ability of the files |
The study of the literature shows that there are conflicting findings regarding the different effects of sterilization procedures. In sum, sterilization and disinfection procedures produce changes in physical and mechanical characteristics, but conclusions about whether the effects are favorable or unfavorable for clinical use are not always consistent between studies.
The alterations can be summarized as follows:
Conceptualization, MD, AD, KZ, RA, GI; methodology, MD and DS; software, GI; validation, MD and AD; formal analysis, MD and AD; investigation, DS and AD and VCAC; resources, LLM; data curation, EL, BR and LL; writing—original draft preparation, MD and GT; writing—review and editing, MD, GT, CA and LLM.
Not applicable.
Not applicable.
This research received no external funding.
The authors declare no conflict of interest.
PRISMA, Preferred Reporting Items for Systematic reviews and Meta-Analyses; SEM, scanning electron microscopy; AFM, atomic force microscopy; AMR, arithmetic mean roughness; MH, maximum height; RMS, root mean square.
