§Alzheimer's Disease Neuroimaging Initiative, Data used in preparation of this article were obtained from the Alzheimer's Disease Neuroimaging Initiative (ADNI) database (adni.loni.usc.edu). As such, the investigators within the ADNI contributed to the design and implementation of ADNI and/or provided data but did not participate in analysis or writing of this report. A complete listing of ADNI investigators can be found at: http://adni.loni.usc.edu/wpcontent/uploads/how_to_apply/ADNI_Acknowledgement_List.pdf
Cerebrospinal fluid neurofilament light and plasma neurofilament light concentrations are elevated in patients with mild cognitive impairment and Alzheimer’s disease. We investigated the clinical relevance of increased neurofilament light concentrations in mild cognitive impairment and Alzheimer’s disease patients. In this study, 244 subjects were divided into cognitively normal control (n = 67), stable mild cognitive impairment (n = 52), progressive mild cognitive impairment (n = 68), and Alzheimer’s disease (n = 57). Linear regression examined the relationships between neurofilament light levels in cerebrospinal fluid or plasma and the diagnostic group. The relationships between neurofilament light and other biomarkers were assessed by Spearman correlation. Linear mixed-effects models were used to test cerebrospinal fluid and plasma neurofilament light as predictors of Alzheimer’s disease characteristics, including cognition, cortical glucose metabolism, and brain structure. Cerebrospinal fluid and plasma neurofilament light levels were significantly elevated in Alzheimer’s disease. Still, the correlations between neurofilament light and other cerebrospinal fluid biomarkers within the diagnostic groups were often not statistically significant. In addition, the diagnostic accuracy of cerebrospinal fluid and plasma neurofilament light for progressive mild cognitive impairment and Alzheimer’s disease was almost the same as that of cerebrospinal fluid total tau (T-tau). It is phosphorylated tau (P-tau) and high cerebrospinal fluid. Neurofilament light predicted conversion from mild cognitive impairment to Alzheimer’s disease. A high neurofilament light is related to poor cognition, low cerebral metabolism, hippocampal atrophy, and ventricular enlargement caused by Alzheimer’s disease. Our work further identifies cerebrospinal fluid neurofilament light and plasma neurofilament light as biomarkers of axonal degeneration in patients with mild cognitive impairment and Alzheimer’s disease.
Alzheimer’s disease (AD) is the main cause of dementia, which is characterized
by extracellular accumulation of aggregated
Neurofilaments are the structural components of axons, which can be measured in
CSF [10, 11]. In CSF, neurofilament proteins (cytoskeletal protein of neurons),
including neurofilament light chain (NFL), were associated with axonal
degeneration in various diseases, including AD [12]. Several reports have
suggested that CSF NFL are elevated early in the AD process and are associated
with longitudinal neurodegeneration and cognitive decline [13]. Interestingly,
recent studies have demonstrated that concentrations of NFL derived from plasma
were elevated in patients with AD and related to CSF A
However, the diagnostic value of CSF NFL or plasma NFL (NFL in plasma) for mild cognitive impairment (MCI) or AD is unclear [14, 17]. Similarly, it is not clear whether the combination of CSF NFL and plasma NFL can improve the diagnostic accuracy of MCI and AD, or whether CSF or plasma NFL forecasts progression from cognitively normal (CN) control to MCI or as from MCI to AD. The purpose of this study is, therefore, to examine the hypotheses that the combination of CSF and plasma NFL improve the diagnostic accuracy for MCI and AD and whether CSF and plasma NFL predict progression from MCI to AD or from CN to MCI or AD in participants enrolled in the Alzheimer’s Disease Neuroimaging Initiative (ADNI) study [18]. We also assess whether CSF or plasma NFL is related to cognitive dysfunction, brain structure, and cerebral metabolism.
Data for this work came from the ADNI database. The subjects participating in this study were between 55 and 90 years old. All subjects completed lumbar puncture, Clinical Dementia Rating scale (CDR), Mini-Mental State Examination (MMSE), and Alzheimer’s Disease Assessment Scale cognitive subscale 11 (ADAS-cog 11) assessments. Furthermore, all participants had magnetic resonance imaging (MRI) and 18F-Fluorodeoxyglucose-positron emission tomography (FDG-PET). Based on clinical and behavioral measurements provided by ADNI, these participants were divided into CN (n = 67), stable MCI (sMCI, n = 52), progressive MCI (pMCI, n = 68), and AD dementia (n = 57).
The CN criteria include MMSE score 26–30 and CDR of 0 [19, 20]. The MCI criteria consisted of subjective memory complaints, MMSE score 24–30, CDR of 0.5, and retained activities of daily living [21]. In addition to the NINCDS/ADRDA criteria, AD individuals had MMSE scores of 20–26 and CDR scores of 0.5 or 1.0 [22]. We referred to MCI subjects who did not progress to AD during a follow-up period of at least 2 years as sMCI and MCI participants who developed to AD at any time during the follow-up period as pMCI [23].
As described previously [24], Multiple xMAP Luminex platforms and Innogenetics
INNO-BIA AlzBio3 immunoassay reagents were used to measure the levels of CSF
A
The baseline data of ADNI PET images were collected and processed according to
the descriptions by Landau et al. [27]. In short, we applied the mean
PET SUVRs in anterior cingulate, lateral and medial frontal lobes, lateral
temporal lobes, lateral parietal, and posterior cingulate [23]. (
Cohort demographics were examined using chi-square analysis and analysis of covariance (ANOVA). Multivariate linear regression was used to measure the relationship between CSF NFL or plasma NFL and clinical diagnostic group, adjusted for age and gender.
The correlation between CSF NFL or plasma NFL and other core biomarkers was examined using Spearman correlation. The overall diagnostic accuracy (area under the receiver operator characteristics curve, AUC) of each biomarker was obtained by Receiver operating curve (ROC) analyses. The difference of AUC between two pairs of different biomarkers was measured using bootstrapping.
To examine the relationship between CSF NFL or plasma NFL and AD dementia, Cox proportional hazard regression analysis (adjusted age and gender) calculated hazard ratios (HR) with 95% CIs. According to the median of each biomarker, CSF NFL and plasma NFL were divided into two groups in Cox proportional hazard regression analyses.
Baseline values of MMSE, ADAS-cog 11, hippocampal and ventricular volumes, and
FDG-PET SUVRs were obtained from the intercepts of linear mixed-effects models.
The intercepts were subsequently used in linear regression models, and the CSF
and plasma NFL values were used as the predictor of clinical diagnostic groups
adjusted for age and gender. MMSE and ADAS-cog-11 analyses were additionally
corrected for education. Hippocampal and ventricular volume analyses were
additionally corrected for intracranial volume. All statistics were conducted
using SPSS version 20 (SPSS Inc., Chicago, IL, USA). The statistical significance
of all analyses was defined as p
The biomarker characteristics and demographics of all subjects are shown in
Table 1. There were no differences in age or education among clinical groups.
There were significantly fewer female individuals in the sMCI group compared to
CN and AD groups. Apolipoprotein E (APOE)
| Characteristics | CN (n = 67) | sMCI (n = 52) | pMCI (n = 68) | AD (n = 57) |
| Age (years) | 75.2 (0.6) | 73.4 (1.1) | 72.9 (0.9) | 74.3 (1.1) |
| Gender (F%) | 30 (44.8%) |
13 (25.0%) |
28 (41.2%) | 28 (49.1%) |
| Education (years) | 15.9 (0.3) | 15.6 (0.4) | 15.9 (0.4) | 15.1 (0.4) |
| APOE ε4 (n%) | 17 (25.4%) |
26 (50.0%) |
44 (64.7%) |
40 (70.2%) |
| Post hoc analysis provided significant differences between groups: | ||||
CSF NFL concentrations in pMCI and AD were higher than that in CN (p
 Fig. 1.
Fig. 1.The levels of CSF and plasma NFL in different groups. The
levels of CSF NFL (A) and plasma NFL (B) in different groups. Differences among
groups were detected by multiple-variable linear regression. *p
CSF NFL related to plasma NFL in all diagnostic groups (Fig. 2A and Table 2).
There was a negative relationship between CSF NFL and A
 Fig. 2.
Fig. 2.CSF NFL in relation to plasma NFL and other biomarkers.
Relationships between CSF NFL and plasma NFL(A) and A
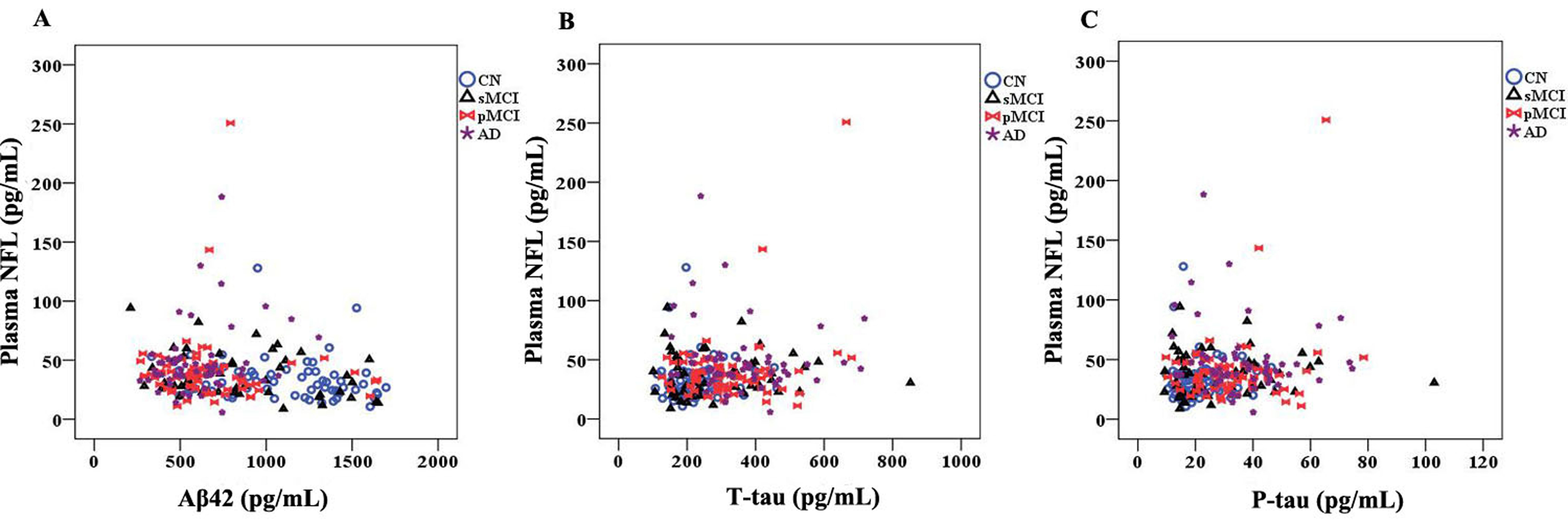 Fig. 3.
Fig. 3.Plasma NFL in relation to other biomarkers. There are
relationships between plasma NFL and A
| CN | sMCI | pMCI | AD | |
| CSF NFL vs Plasma NFL | r = 0.514 (p |
r = 0.603 (p |
r = 0.530 (p |
r = 0.371 (p = 0.005) |
| CSF NFL vs CSF A |
r = –0.245 (p = 0.046) | r = 0.001 (p = 0.996) | r = 0.195 (p = 0.109) | r = 0.237 (p = 0.076) |
| CSF NFL vs CSF T-tau | r = 0.514 (p |
r = 0.094 (p = 0.502) | r = 0.049 (p = 0.687) | r = 0.284 (p = 0.032) |
| CSF NFL vs CSF P-tau | r = 0.472 (p |
r = 0.052 (p = 0.711) | r = –0.031 (p = 0.799) | r = 0.284 (p = 0.063) |
| Plasma NFL vs CSF A |
r = –0.125 (p = 0.313) | r = –0.044 (p = 0.752) | r = 0.030 (p = 0.805) | r = 0.247 (p = 0.065) |
| Plasma NFL vs CSF T-tau | r = 0.076 (p = 0.543) | r = –0.020 (p = 0.885) | r = 0.285 (p = 0.018) | r = –0.132 (p = 0.327) |
| Plasma NFL vs CSF P-tau | r = 0.042 (p = 0.737) | r = –0.047 (p = 0.738) | r = 0.202 (p = 0.097) | r = –0.142 (p = 0.292) |
ROC analyses were used to detect CSF biomarkers associated with sMCI, pMCI, and AD clinical diagnoses. Except for the combination of CSF NFL and plasma NFL, other biomarkers did not have significantly different diagnostic accuracy for sMCI (Fig. 4A and Table 3). All biomarkers had significant accuracy in diagnosing pMCI (Fig. 4B and Table 3) and AD (Fig. 4C and Table 3). CSF T-tau and P-tau, CSF NFL and plasma NFL had almost the same diagnostic accuracy in pMCI and AD (Fig. 4B,C and Table 3).
| CSF NFL | Plasma NFL | CSF and Plasma NFL | T-tau | P-tau | |
| CN vs sMCI | 0.604 (0.501–0.706) (p = 0.053) | 0.575 (0.470–0.681) (p = 0.159) | 0.613 (0.510–0.715) (p = 0.036) | 0.578 (0.469–0.687) (p = 0.146) | 0.592 (0.484–0.699) (p = 0.087) |
| CN vs pMCI | 0.719 (0.632–0.805) (p |
0.630 (0.536–0.724) (p = 0.009) | 0.716 (0.629–0.803) (p |
0.775 (0.695–0.854) (p |
0.781 (0.701–0.860) (p |
| CN vs AD | 0.760 (0.676–0.844) (p |
0.728 (0.638–0.818) (p |
0.781 (0.702–0.861) (p |
0.811 (0.733–0.889) (p |
0.811 (0.732–0.891) (p |
 Fig. 4.
Fig. 4.ROC analyses. ROC analyses were used to assess the CSF biomarkers associated with clinical diagnoses for sMCI (A), pMCI (B), and AD (C).
17 CN participants progressed to MCI or AD dementia during the follow-up period,
and 68 MCI patients developed AD dementia. We tested whether baseline
concentrations of CSF NFL and plasma NFL predicted conversion from CN to MCI or
AD dementia and from MCI to AD dementia. CSF NFL and plasma NFL were used as
continuous variables to establish Cox proportional hazard models. CSF NFL did not
significantly predict conversion from CN to MCI or AD dementia (Fig. 5A).
However, individuals with high CSF NFL, corresponding to MCI individuals whose
CSF NFL were
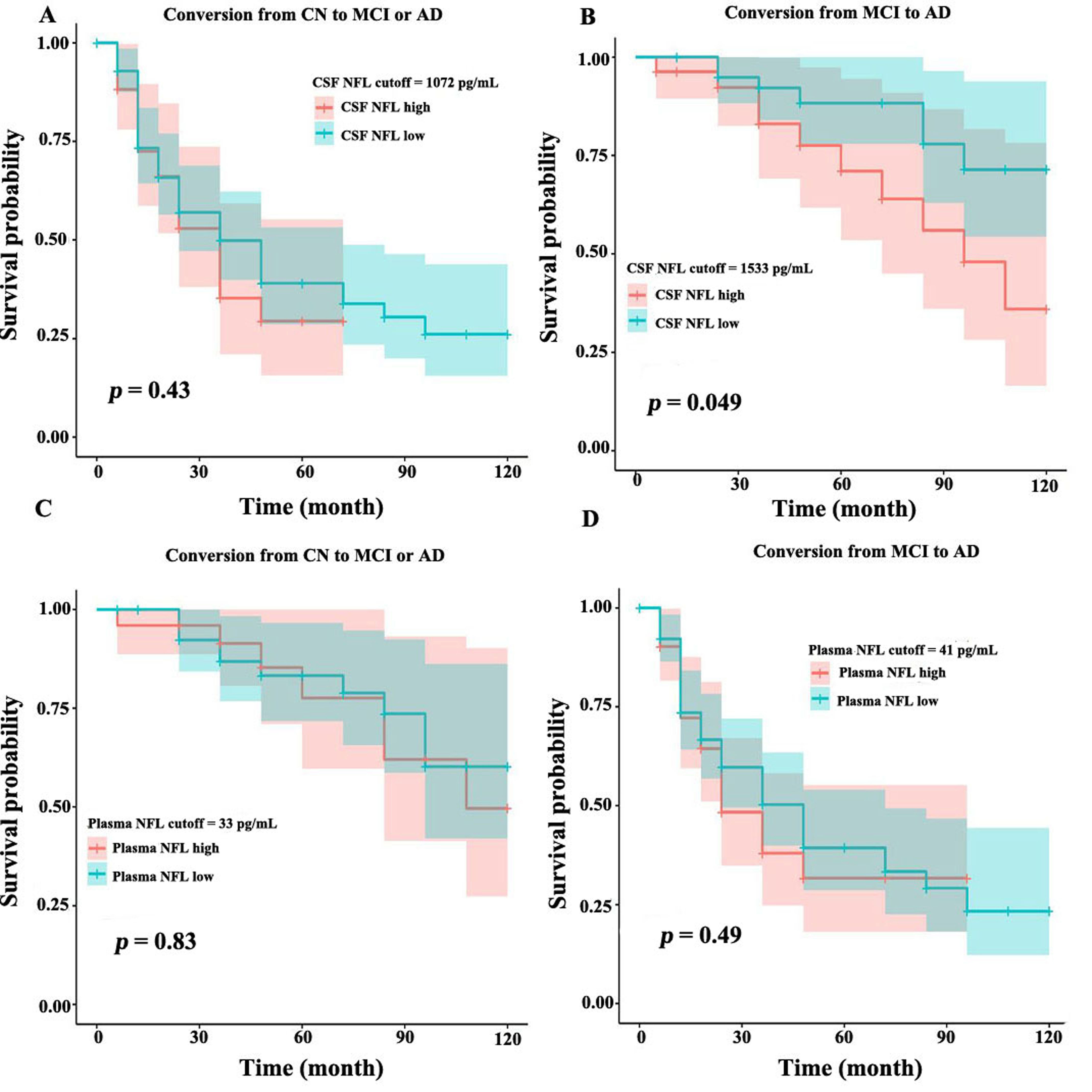 Fig. 5.
Fig. 5.Baseline CSF and plasma NFL as predictors of conversion from CN to MCI or AD and MCI to AD. Conversion from CN to MCI or AD (A) and MCI to AD (B) as a function of CSF NFL. Conversion from CN to MCI or AD (C) and MCI to AD (D) as a function of plasma NFL.
High CSF NFL related to low MMSE (
 Fig. 6.
Fig. 6.CSF and plasma NFL in relation to baseline cognition. MMSE (A) and ADAS-Cog (B) at baseline function as baseline CSF NFL in different groups. MMSE (C) and ADAS-Cog (D) at baseline function as baseline plasma NFL in different groups. Values of all indicators are normalized.
CSF NFL correlated with baseline FDG-PET in CN (
 Fig. 7.
Fig. 7.CSF and plasma NFL in relation to baseline metabolism and brain structure. FDG (A), hippocampal volumes (B), and ventricular volumes (C) at baseline as a function of baseline CSF NFL in different groups. FDG (D), hippocampal volumes (E), and ventricular volumes (F) at baseline as a function of baseline plasma NFL in different groups. Values of all indicators are normalized.
Plasma NFL correlated with baseline FDG-PET in CN (
We evaluated the relationships between CSF and plasma NFL in MCI and AD patients from the ADNI database. We have the following major findings: firstly, CSF and plasma NFL concentrations were significantly elevated in AD. CSF NFL, but not plasma NFL, was significantly increased in pMCI relative to CN. Secondly, CSF and plasma NFL had almost the same diagnostic accuracy as CSF T-tau and P-tau for pMCI and AD. Our third main finding is that individuals with high CSF NFL progressed much more rapidly to AD than subjects with lower levels. Finally, CSF and plasma NFL are associated with baseline cognition in sMCI and AD and baseline cerebral metabolism and brain structure at some stages of AD.
In line with a previous study [13], we report that CSF NFL was significantly
higher in pMCI and AD dementia than CN individuals. We also observed there were
significant differences between sMCI and AD. However, contrary to some existing
reports [14, 15, 17], plasma NFL in our study was significantly different between
CN and AD and between sMCI and AD. Still, there were no significant differences
among CN, sMCI, and pMCI. One explanation for these differences is that the
number of cases in our study is relatively small, and the sampling bias is large.
Moreover, in the present study, the correlations between CSF and plasma NFL with
other CSF biomarkers were usually not statistically significant in the diagnostic
groups. This finding may confirm the presence of several different pathological
conditions in AD (such as A
In our study, compared with CSF T-tau and P-tau, CSF and plasma NFL had almost the same diagnostic accuracy for pMCI and AD. However, CSF and plasma NFL combined did not significantly improve the diagnostic accuracy for pMCI and AD over either biomarker in isolation. Interestingly, the combination of CSF and plasma NFL provided significantly different diagnostic accuracy for sMCI in our study, but CSF NFL, plasma NFL, CSF T-tau, and CSF P-tau had no similar effects, indicating that the combination of CSF and plasma NFL may be useful for the diagnosis of prodromal stages of AD. In the future, we should verify its specificity for the diagnosis of sMCI in other neurodegenerative diseases.
There is increasing evidence that axonal degeneration is a surrogate indicator
of AD neurodegeneration progression [1, 28]. Although it has been shown that the
combination of plasma NFL and MMSE could reliably predict whether MCI patients
might progress to AD dementia within 5 years [29]. To our knowledge, no studies
using Cox proportional hazard models have evaluated the predictive value of CSF
NFL for the conversion from CN to MCI or AD and from MCI to AD. Here, we
demonstrate that CSF NFL but not plasma NFL provides predictive value for future
disease progression in MCI participants. Our findings indicate that CSF NFL may
contribute to the prognostic roles of CSF A
Previous research has reported that plasma NFL might be a promising biomarker of progressive cognitive decline in elderly patients with MCI [30]. We examined the associations between CSF or plasma NFL and cognition. Statistically significant interactions were found at baseline for the sMCI group and MMSE or ADAS-cog 11 and the AD group and MMSE or ADAS-cog 11. These results suggest that CSF and plasma NFL were more strongly associated with the cognitive outcomes in sMCI and AD than in CN at baseline. It has been shown that in the MCI group, higher CSF NFL concentrations were related to faster brain atrophy over time, as measured by changes in whole-brain volume, ventricular volume, and hippocampal volume [13]. In addition, Mattsson et al. [14] reported that elevated plasma NFL was associated with AD-related atrophy (baseline and overtime) and brain hypometabolism (over time).
Our results show that CSF and plasma NFL were correlated with several baseline imaging measures of AD-related neurodegeneration, including low cortical glucose metabolism, hippocampal atrophy, and ventricular enlargement. These relationships were particularly pronounced with CSF and plasma NFL in relation to large ventricles in CN, sMCI, and AD groups. These results indicate that AD’s cognition, brain structure, and cortical metabolism may be related to axonal degeneration. However, there were some inconsistencies in the correlation between NFL and cognition and between NFL and brain metabolism or structure. For example, the correlations between MMSE or ADAS-Cog and CSF or plasma NFL in pMCI patients were the opposite of all other groups.
Similarly, brain metabolism correlated well with plasma NFL in CN and sMCI but not in pMCI and AD. Vice versa CSF NFL correlated well with baseline FDG brain metabolism in CN and AD, but not in pMCI and sMCI, suggesting that they were confounded by diagnosis. We do not know the exact reason, but it indicates that cognition, brain metabolism, and brain structure may be related to many factors, and NFL is only one of them.
CSF and plasma NFL concentrations are significantly higher in other neurodegenerative diseases other than AD than healthy controls [28, 31, 32, 33, 34]. In addition, although a previous study investigated that CSF NFL had the potential to help distinguish frontotemporal dementia from AD and Parkinson disease from atypical Parkinson’s syndrome [34], the diagnostic usefulness of CSF and plasma NFL might be limited due to the finding that it is also elevated in other neurodegenerative diseases, indicating low specificity for AD.
Our results support the use of NFL as a biomarker of axonal degeneration. CSF and plasma NFL were significantly elevated in AD. In addition, compared with CSF T-tau and P-tau, CSF and plasma NFL had similar diagnostic accuracy for pMCI and AD. Moreover, high CSF NFL predicted conversion from MCI to AD. Finally, high CSF and plasma NFL are related to poor cognition, low metabolism, hippocampal atrophy, and ventricular enlargement at some stages of AD. These findings may suggest the potential use of NFL in trial designs, monitoring response to therapies, treatment decisions, and outcome evaluations.
A
YC—manuscript drafting. JT—manuscript drafting. JL—analysis of data. MB—analysis and interpretation of data. HZ—critical review of manuscript and study supervision.
The Institutional Review Boards of all participating institutions approved the ADNI study. All participants in each centre obtained informed written consent. ADNI makes all its data publicly available. Our manuscript was approved and accepted for submission by the ADNI Data and Publications Committee (ADNI DPC). For more details, please see: http://adni.loni.usc.edu/data-samples/access-data/.
Data collection and sharing for this project was funded by the Alzheimer’s Disease Neuroimaging Initiative (ADNI) (National Institutes of Health Grant U01 AG024904) and DOD ADNI (Department of Defense award number W81XWH-12-2-0012). ADNI is funded by the National Institute on Aging, the National Institute of Biomedical Imaging and Bioengineering, and through generous contributions from the following: AbbVie, Alzheimer’s Association; Alzheimer’s Drug Discovery Foundation; Araclon Biotech; BioClinica, Inc.; Biogen; Bristol-Myers Squibb Company; CereSpir, Inc.; Cogstate; Eisai Inc.; Elan Pharmaceuticals, Inc.; Eli Lilly and Company; EuroImmun; F. Hoffmann-La Roche Ltd and its affiliated company Genentech, Inc.; Fujirebio; GE Healthcare; IXICO Ltd.; Janssen Alzheimer Immunotherapy Research & Development, LLC.; Johnson & Johnson Pharmaceutical Research & Development LLC.; Lumosity; Lundbeck; Merck & Co., Inc.; Meso Scale Diagnostics, LLC.; NeuroRx Research; Neurotrack Technologies; Novartis Pharmaceuticals Corporation; Pfizer Inc.; Piramal Imaging; Servier; Takeda Pharmaceutical Company; and Transition Therapeutics. The Canadian Institutes of Health Research is providing funds to support ADNI clinical sites in Canada. Private sector contributions are facilitated by the Foundation for the National Institutes of Health (www.fnih.org). The grantee organization is the Northern California Institute for Research and Education, and the study is coordinated by the Alzheimer’s Therapeutic Research Institute at the University of Southern California. ADNI data are disseminated by the Laboratory for Neuro Imaging at the University of Southern California.
This study was supported by the Medical Research Project of Chongqing Healthy Committee (2018MSXM058).
The authors declare no conflict of interest.
