Background: This study aimed to evaluate the effectiveness of pelvic
and para-aortic lymphadenectomy in patients with advanced epithelial ovarian
cancer following neoadjuvant chemotherapy. Methods: This single-center
retrospective study analyzed patients with advanced epithelial ovarian cancer who
underwent interval debulking surgery between December 2008 and March 2020.
Patients’ clinical and pathological data were obtained from medical records.
Statistical analyses were performed using the Fisher’s exact and Mann–Whitney U
test. Results: Overall, 33 and 22 patients were included in the
lymphadenectomy and no-lymphadenectomy groups, respectively. The lymphadenectomy
group had longer operative time and higher rates of intraoperative blood loss and
lymph cysts than the no-lymphadenectomy group (p 0.0001). The median
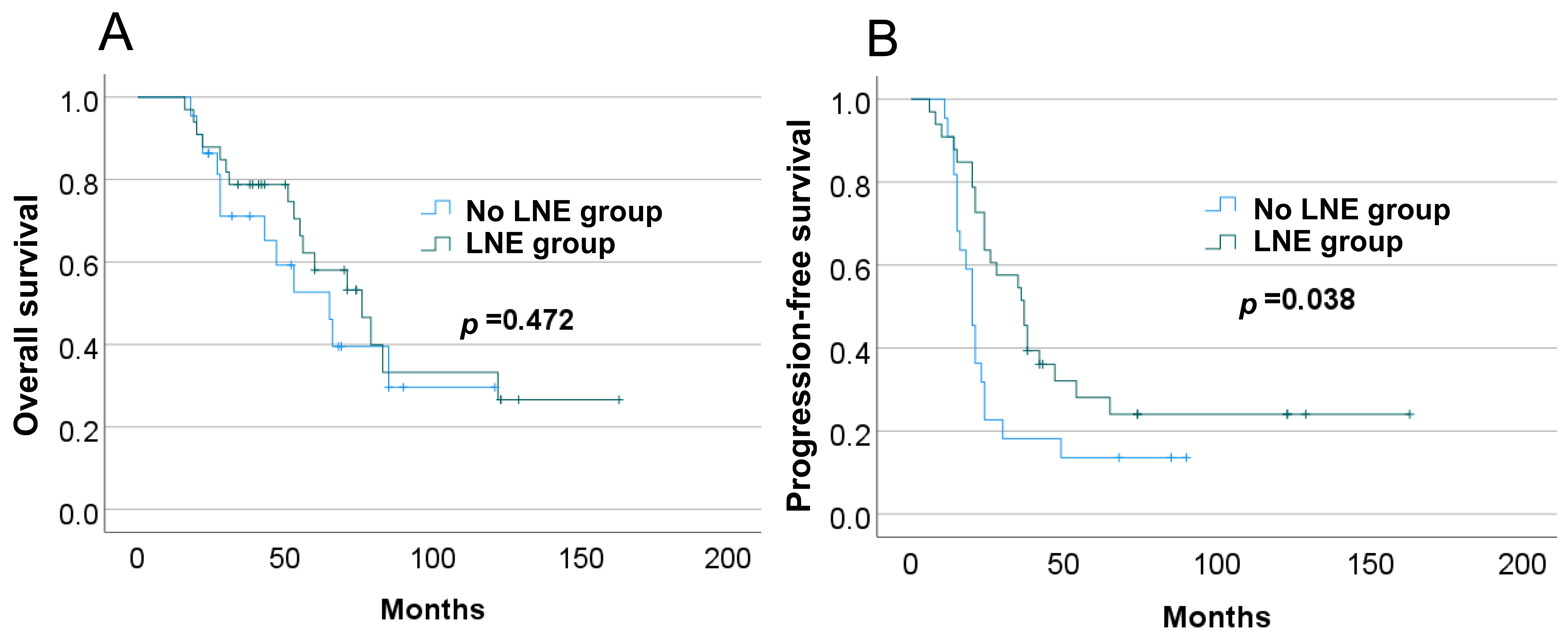
progression-free survival (PFS) was longer in the lymphadenectomy group than in
the no-lymphadenectomy group (37.0 vs. 20.0 months, p = 0.038).
Among patients with enlarged lymph nodes before chemotherapy, the median PFS was
longer in the lymphadenectomy group than in the no-lymphadenectomy group (36.0
vs. 15.0 months, p = 0.013). Multivariate analysis of all
patients revealed that residual tumor status (p = 0.002) and histology
(p = 0.009) were associated with PFS. Additionally, multivariate
analysis of patients with enlarged lymph nodes before chemotherapy showed that
lymphadenectomy (p = 0.017) and histology (p = 0.021) were
associated with PFS. Conclusions: Systematic lymphadenectomy was
associated with complications; however, PFS was significantly prolonged in
patients with enlarged lymph nodes in the lymphadenectomy group. Therefore,
lymphadenectomy has the potential to improve prognosis in patients with ovarian
cancer and enlarged lymph nodes.