Background: Metabolic disorders, including obesity, are often
accompanied by an increased risk of cardiovascular complications. Monocytes are
the common link between obesity and cardiovascular diseases (CVDs). The bias of
innate cellular immunity towards pro-inflammatory activation stimulates the
development of diseases associated with chronic inflammation, in particular
metabolic disorders, including obesity, as well as CVDs. Disorders in the
functional state of monocytes and activation of inflammation may be associated
with mitochondrial dysfunction. Mutations accumulating in mitochondrial DNA with
age may lead to mitochondrial dysfunction and may be considered a potential
marker for developing chronic inflammatory diseases. Methods: The
present study aimed to study the relationship between mitochondrial heteroplasmy
in CD14 monocytes and cardiovascular risk factors in 22 patients with
obesity and coronary heart disease (CHD) by comparing them to 22 healthy
subjects. Results: It was found that single-nucleotide variations (SNV)
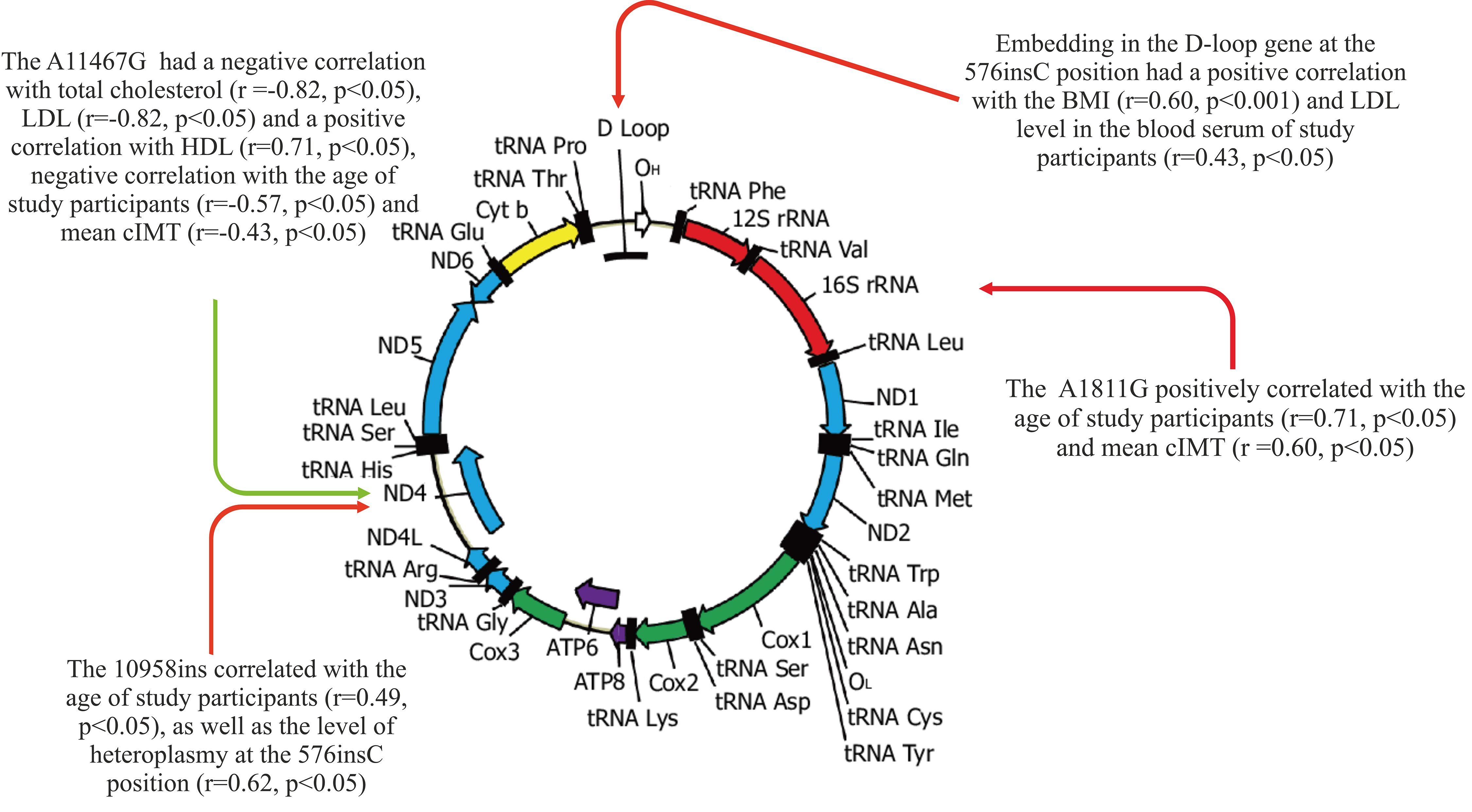
A11467G have a negative correlation with total cholesterol (r = –0.82,
p 0.05), low density lipoproteins (LDL) (r = –0.82, p
0.05), with age (r = –0.57, p 0.05) and with mean carotid
intima-media thickness (cIMT) (r = –0.43, p 0.05) and a positive
correlation with HDL level (r = 0.71, p 0.05). SNV 576insC
positively correlated with body mass index (BMI) (r = 0.60, p 0.001)
and LDL level (r = 0.43, p 0.05). SNV A1811G positively correlated
with mean cIMT (r = 0.60, p 0.05). Conclusions: It was
revealed that some variants of mitochondrial DNA (mtDNA) heteroplasmy are
associated with CVD risk factors. The results demonstrate the potential for using
these molecular genetic markers to develop personalized CVD and metabolic
disorder treatments.